The aim of this study is to investigate the radiological features of primary pulmonary invasive mucinous adenocarcinoma (IMA) in a relatively large population to help improve its further understanding and its accuracy of initial diagnosis.
This retrospective study included consecutive patients with pathologically confirmed primary pulmonary IMA from January 2019 to December 2021. According to tumor morphology, IMAs were divided into regular nodule/mass, irregular, and large consolidative types. According to tumor density, IMAs were divided into solid, halo, part-solid, pure ground-glass, and cystic types. ANOVA, chi-square, or Fisher exact tests were used to analyze the differences in radiological and clinicopathological characteristics of IMA according to morphological and density subtypes.
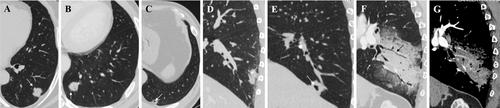
We analyzed 312 patients. Pulmonary IMA tended to occur in the elderly, with a slightly higher number of women than men. IMA showed a predominance in the lower lobe and adjacent to pleura. IMA of regular nodule/mass, irregular, and large consolidative types accounted for 80.8% (252/312), 13.8% (43/312), and 5.4% (17/312), respectively. Solid, halo, part-solid, pure ground-glass, and cystic IMAs accounted for 55.8% (174/312), 28.2% (88/312), 11.2% (35/312), 1.3% (4/312), and 3.5% (11/312), respectively. The lobulated (76.9%), spiculated (63.5%), and air bronchogram (56.7%) signs were common in IMA. Dead branch sign (88.2%), angiogram sign (88.2%), and satellite nodules/skipping lesions (47.1%) were common in large-consolidative-type IMA. Kirsten rat sarcoma viral oncogene mutations were common (56.1%), whereas epidermal growth factor receptor mutations were relatively rare (2.3%).
Pulmonary IMA of regular nodule/mass type and solid type were the most common at the initial diagnosis. Detailed radiological features can aid in the differential diagnosis of IMA.