Polycystic ovarian syndrome (PCOS) is the commonest endocrine condition affecting reproductive age women. Many biomarkers may aid assessment and management, however evidence is limited on their utility in clinical practice. We conducted a review of systematic reviews to identify the most useful biomarkers in the clinical management of PCOS.
We searched MEDLINE, EMBASE, CENTRAL and HTA until August 2023 for reviews evaluating biomarkers in PCOS women compared to healthy controls. Methodological quality was assessed using the AMSTAR2 tool. We reported pooled evidence for each biomarker with 95% confidence intervals from the most recent, up-to-date, and best quality review.
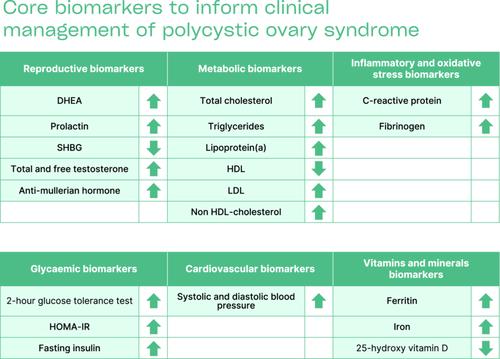
From 3360 citations, we included 75 systematic reviews (88 biomarkers, 191,792 women). Most reviews (50/75, 67%) were moderate quality, but reported high heterogeneity (66/75, 88%). We identified 63 abnormal biomarkers in women with PCOS versus healthy controls. Of these, 22 core biomarkers could help evaluate the multisystemic impact of PCOS and inform patient management and surveillance: dehydroepiandrosterone, prolactin, sex hormone-binding globulin, total and free testosterone, anti-Mullerian hormone, systolic and diastolic blood pressure, c-reactive protein, fibrinogen, oral glucose tolerance test, homoeostatic model assessment-insulin resistance index, fasting insulin, total cholesterol, triglycerides, lipoprotein(a), HDL, LDL, non-HDL-cholesterol, ferritin, iron, and 25-hydroxy-vitamin D.
We identified 22 core biomarkers assessing the multisystemic impact of PCOS and inform its clinical management. Future research is required to establish validated healthcare pathways.