The establishment of midwife-led birth centers (MLBCs) is still being debated. The study aimed to compare severe adverse outcomes and mode of birth in low-risk women according to their birth planned in MLBCs or in obstetric-led units (OUs) in France.
We used nationwide databases to select low-risk women at the start of care in labor in MLBCs (n = 1294) and in OUs (n = 5985). Using multilevel logistic regression, we compared severe adverse maternal and neonatal morbidity as a composite outcome and as individual outcomes. These include severe postpartum hemorrhage (≥1000 mL of blood loss), obstetrical anal sphincter injury, maternal admission to an intensive care unit, maternal death, a 5-minute Apgar score <7, neonatal resuscitation at birth, neonatal admission to an intensive care unit, and stillbirth or neonatal death. We also studied the mode of birth and the role of prophylactic administration of oxytocin at birth in the association between birth settings and severe postpartum hemorrhage.
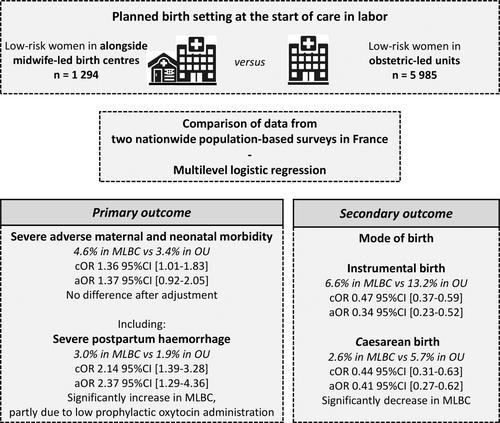
Severe adverse maternal and neonatal outcome indicated a slightly higher rate in women in MLBCs compared to OUs according to unadjusted analyses (4.6% in MLBCs vs. 3.4% in OUs; cOR 1.36; 95%CI [1.01–1.83]), but the difference was not significant between birth settings after adjustment (aOR 1.37 [0.92–2.05]). Severe neonatal morbidity alone was not different (1.7% vs. 1.6%; aOR 1.17 [0.55–2.47]). However, severe maternal morbidity was significantly higher in MLBCs than in OUs (3.0% vs. 1.9%; aOR 1.61 [1.09–2.39]), mainly explained by higher risks of severe postpartum hemorrhage (2.4 vs. 1.1%; aOR 2.37 [1.29–4.36]), with 2 out of 5 in MLBCs partly explained by the low use of prophylactic oxytocin. Cesarean and operative vaginal births were significantly decreased in women with a birth planned in MLBCs.
In France, 3 to 4% of low-risk women experienced a severe adverse maternal or neonatal outcome regardless of the planned birth setting. Results were favorable for MLBCs in terms of mode of birth but not for severe postpartum hemorrhage, which could be partly addressed by revising practices of prophylactic administration of oxytocin.