Identifying the likelihood of life-threatening recurrence after radical cystectomy by reliable and user-friendly predictive models remains an unmet need in the clinical management of invasive bladder cancer.
A total of 204 consecutive patients undergoing open radical cystectomy (ORC) for bladder cancer were retrospectively enrolled between May 2005 and August 2020. Clinicopathological and peri-ORC therapeutic data were extracted from clinical records. We explored predictive factors that significantly affected the primary endpoint of overall survival (OS) and secondary endpoints of cancer-specific survival (CSS) and recurrence-free survival (RFS).
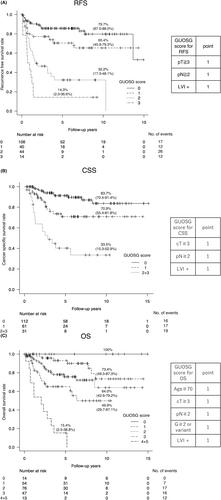
During a median follow-up of 3.9 years, 42 (20.6%) and 10 (4.9%) patients died due to bladder cancer and other causes, respectively. Five-year RFS, CSS, and OS were 66.5%, 77.6%, and 75.4%, respectively. Pathological T and N categories and lymphovascular invasion (LVI) significantly affected RFS by Cox regression analysis. Accordingly, clinical T and pathological N categories and LVI significantly affected CSS. Clinical T and pathological N categories, LVI, age, and ORC tumor grade significantly affected OS. Based on the assessment score for each independent risk factor, we developed the Gunma University Oncology Study Group (GUOSG) score, which predicts RFS, CSS, and OS. The GUOSG score classified four groups for RFS, three for CSS, and five for OS, with statistically significant distribution for nearly all comparisons.
The GUOSG model is helpful to show individualized prognosis and functions as a risk-stratified historical cohort for assessing the lifelong efficacy of new salvage treatment regimens.